Fixing the Bridge in Revision Rhinoplasty: Dorsal Augmentation with Grated Cartilage Composite Graft
March 22, 2026 | Revision Rhinoplasty
8 Minute Read
Patients seeking revision rhinoplasty most commonly have concerns about two major anatomic regions: the bridge — known in medical terminology as the dorsum — and the tip. This blog addresses an innovative method for correcting dorsal abnormalities. A separate blog covering tip correction in revision rhinoplasty will follow.
Dorsal problems in revision rhinoplasty are not all the same. Understanding the type of abnormality is the first step toward selecting the right solution.
Table of Contents
- The Three Presentations of Dorsal Abnormality
- When Dorsal Augmentation Is Needed
- Alloplastic Implants: Why They’ve Largely Been Abandoned
- Costal Cartilage: The Current Standard
- Grated Cartilage Composite Grafting: My Approach
- Surgical Technique Video
- Before and After
The Three Presentations of Dorsal Abnormality
Problems with the nasal bridge generally come in three forms — and in some patients, these presentations overlap. The three categories are:
- Over-projected dorsum: The height of the bridge is greater than the patient desires.
- Under-projected dorsum: The bridge does not project enough — often the result of over-resection of bone and cartilage during a prior surgery.
- Irregular dorsal surface: The bridge is at an appropriate height, but the surface has significant irregularities — lumps, bumps, peaks and valleys, changes in width, or deviation to one side due to a tilted septum or asymmetric bone and upper lateral cartilage anatomy.
Over-projection is actually the more favorable situation in terms of correction. Because there is ample bone and cartilage to work with, the dorsum can typically be reduced and smoothed without importing any additional material. In contrast, under-projected dorsa and severely irregular dorsal surfaces cannot be corrected using the existing tissue alone — by definition, there is a shortage of acceptable bone and cartilage. That is where the importation of material — and in most practices today, the importation of cartilage specifically — becomes necessary. This process is called dorsal augmentation.
When Dorsal Augmentation Is Needed
Dorsal augmentation is useful not only in revision rhinoplasty, but also in primary rhinoplasty for patients from ethnicities whose noses are characterized by under-projection — generally patients of African or African-American, Asian, or some Latino ancestry who desire increased bridge projection. The technique and the principles are similar across both contexts.
Alloplastic Implants: Why They’ve Largely Been Abandoned
Alloplastic implants — meaning synthetic, non-biological implants — have been used for dorsal augmentation in the past. The two main types are silicone implants, which are moderately flexible but maintain their shape, and firm plastic implants such as porous polyethylene. Both are placed beneath the skin on top of the remaining bone and cartilage of the upper two-thirds of the nose.
For the most part, these methods have been abandoned by most plastic surgeons due to a number of problems: shifting of the implant over time, infection, and even exposure — meaning the implant can work its way through the thin skin of the nose. These complications make alloplastic implants a poor choice, particularly in revision rhinoplasty where tissue quality and vascularity may already be compromised.
Costal Cartilage: The Current Standard
Because alloplastic implants are now rarely used, the majority of dorsal augmentation relies on costal cartilage — meaning rib cartilage. There are two sources:
- Autologous costal cartilage: Cartilage harvested from the patient’s own ribs and relocated to the nose. In my practice, this is harvested from the right side of the chest through an incision that is less than one inch long in patients of normal weight. In women, this incision is typically placed just beneath the inframammary fold — where the breast meets the chest wall. In men, the location is somewhat more variable, but I aim for what I call the “sweet spot” — an area where the rectus abdominis, the pectoralis major, and the serratus anterior all meet at a junction that allows easy access to the rib without requiring any cutting of muscle fibers. In women with breast implants, special care is taken to avoid any exposure of or contact with the implant.
- Cadaveric rib cartilage: Cartilage harvested from donors who have passed away and donated their tissues. These tissues are processed at specialized facilities and treated in various ways to preserve the tissue and address potential transmission of bacteria or viruses.
Historically, costal cartilage has been used in two main forms for dorsal augmentation: solid carved grafts and diced cartilage wrapped in fascia (DCF). Solid grafts involve carving a large piece of cartilage into the appropriate size and shape, then placing it beneath the skin and holding it in position with sutures or temporary transcutaneous wires. The concern with solid grafts is the potential for warping or shifting over time. DCF — where cartilage is diced into approximately one-to-two millimeter pieces and then wrapped in fascia harvested from the temporalis muscle through an incision in the hair-bearing temple — addresses some of those concerns, but can result in lack of definition and poorly defined dorsal aesthetic lines.
Grated Cartilage Composite Grafting: My Approach
I developed the concept of grated cartilage grafting after reflecting on the limitations of alloplastic implants, solid cartilage grafts, and DCF. My mentor, Dr. Bahman Guyuron, had articulated the wish for a method that would produce small pieces of cartilage — similar to dicing — but in a simpler and more controlled fashion. I arrived at the idea while using various grater devices for household purposes. I identified a specific microplane grater made of surgical-grade steel, and for the past ten years have used grated cartilage composite grafts in over 200 patients.
This technique has served patients well across several clinical contexts: patients from ethnicities requiring dorsal augmentation, patients undergoing cleft rhinoplasty, and particularly patients undergoing revision rhinoplasty who need dorsal resurfacing or augmentation.
The process involves grating the cartilage into small pieces, assembling those pieces in a mold fashioned from a three-part syringe, and bonding the cartilage together with a surgical fibrin sealant glue. The resulting composite can then be carved into the appropriate shape for placement. The video below demonstrates the key steps of this technique.
Over ten years of experience with this method, complication rates have been very low, and the need for revision due to cartilage absorption has been minimal. One additional property worth noting: the portion of a cartilage graft that overlies bone tends to take on increasingly bone-like behavior over time — becoming quite firm — while the portion overlying the cartilaginous components of the nose remains more flexible and mobile. This mimics the natural behavior of the nasal dorsum and contributes to a result that feels as natural as it looks.
Surgical Technique Video
The following video demonstrates the key maneuvers involved in creating the grated cartilage composite graft.
Before and After
The following images show representative patient results following revision rhinoplasty with grated cartilage composite dorsal grafting.
Right Side View
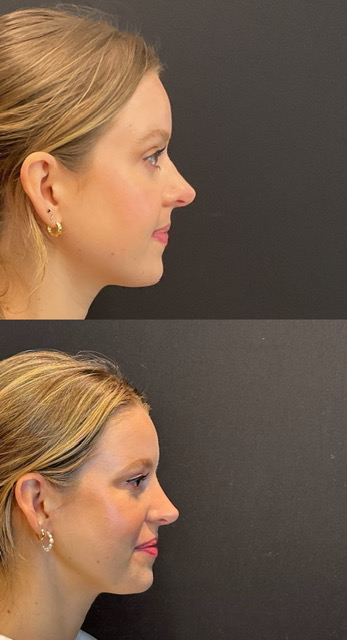
Left Oblique View

Front View

