Deep Plane vs. High SMAS Facelift: What’s the Real Difference?
April 18, 2026 | Facelift
“`
The Science
A patient one day after her deep plane facelift asks about the SMAS — prompting a discussion on how deep plane and high SMAS facelifts compare.
There’s not a common language that people use consistently when describing facelift anatomy and what’s actually done technique-wise. The original description of a deep plane facelift is what many people still call a deep plane facelift today. It’s where you enter the sub-SMAS plane and then dissect the tissue. In the deep plane facelift, this entry is made over the malar eminence — the cheekbone just below the lateral aspect of the eye — and over the gonial angle, where the jawbone transitions from horizontal to vertical. The dissection follows a pretty much linear path between these two points. One of the benefits of this approach is that there is slightly less skin elevation required — and what skin is elevated involves the easier dissection — and then you enter the SMAS where it’s a little bit easier to enter and dissect. There’s actually less dissection underneath the SMAS than is otherwise necessary, and you can elevate the tissues in a more direct way because you’re closer to the tissue that really needs to be repositioned at a deeper level.
A high SMAS facelift, by contrast, means entering the SMAS through a vertical incision that begins near the ear and then continues horizontally across the zygomatic arch — the cheekbone. This entry point is more lateral compared to the deep plane entry, which is why the dissection that follows requires lifting a greater amount of the fixed SMAS before reaching the mobile tissue that needs to be repositioned. With a high SMAS facelift, you do end up dissecting down and then continuing beneath the SMAS, sometimes all the way to the nasolabial fold.
What makes a high SMAS facelift more technically demanding is that you end up lifting a lot of the SMAS in the region of the fixed SMAS — an area where elevation isn’t necessarily required to reposition the target tissue. With a deep plane facelift, the sutures that secure the repositioned tissue originate closer to the deep plane itself, elevated with a span up to the deeper, thicker tissues. With a high SMAS facelift, the sutures tend to be a bit closer to where they’re secured but somewhat more remote from the tissue that most needs to be repositioned.
There are also other SMAS-based techniques worth mentioning. A SMAS plication involves lifting the skin and then folding the SMAS at the junction of the fixed and mobile SMAS — bunching it and suturing it together. It does lift the cheek, but with less range and a less vertical vector than I think is ideal. A SMASectomy is similar in skin elevation but instead of folding the SMAS, a strip is excised and the edges are sutured together. Both are legitimate variations, but they are more limited in what they can achieve.
Suspension Sutures & Shape in the Deep Plane Facelift
In this short, I walk through the suspension suture technique I use to create shape during a deep plane facelift. These same techniques can be modified for the high SMAS facelift as well — which is part of what supports the idea that the two procedures are converging, and that technique needs to be customized for each individual patient.
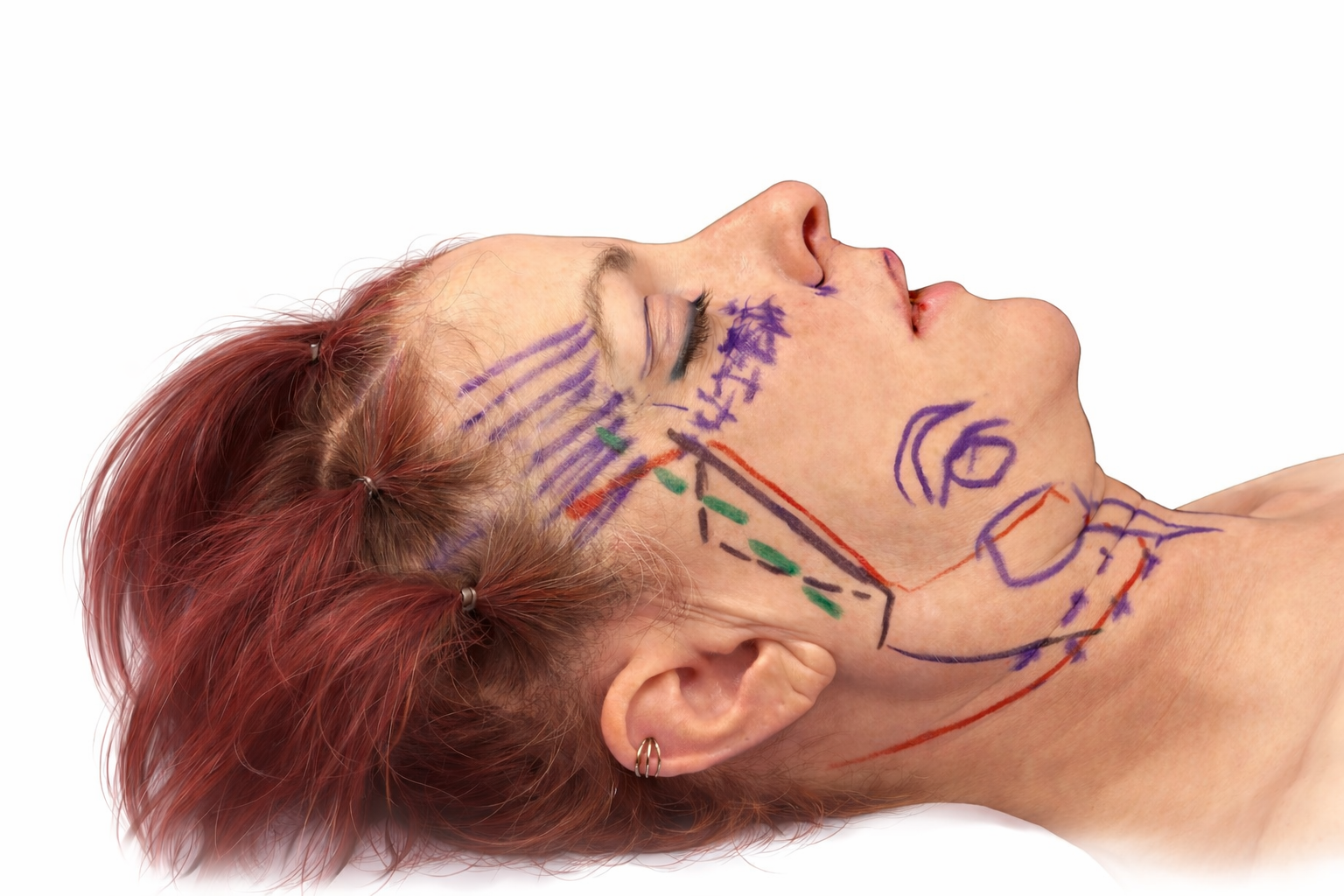
Preoperative markings for a Trimax deep plane facelift with dual plane neck lift. The solid black line marks traditional deep plane entry; the dotted line reflects a high SMAS variant. Red lines outline the skin elevation zone. Plus marks on the cheeks and neck indicate fat grafting sites (including necklace lines). Straight lines in the temple mark additional fat grafting. Micro-liposuction of the jowl is shown along the jaw, and the circle beneath the jawline marks the submandibular gland reduction site. Rendered from an actual patient photograph; background has been simplified using AI for visual clarity.
Preoperative Markings: Understanding Gravity Before Surgery
Before every deep plane facelift, I mark the patient in the upright seated position. This is essential — it allows me to understand how gravity is acting on the soft tissues before the patient is reclined on the operating table. The markings guide where the deep tissue needs to be repositioned to restore a natural, youthful result.
| Deep Plane Facelift | High SMAS Facelift | |
|---|---|---|
| SMAS Entry | Over malar eminence and gonial angle — linear path between the two | Vertical incision near ear, continuing horizontally across the zygomatic arch |
| Entry Location | More medial — closer to the tissue that needs repositioning | More lateral — further from the target tissue |
| Skin Elevation | Slightly less skin elevation required | Greater skin elevation; allows more skin excision |
| Fixed SMAS | Less fixed SMAS elevated — more efficient dissection | More fixed SMAS must be elevated to reach mobile tissue |
| Suture Origin | Closer to the deep plane; spans to deeper, thicker tissue | Closer to where secured, but more remote from the tissue needing most repositioning |
| Sub-SMAS Extent | More limited and targeted dissection | Can extend all the way to the nasolabial fold |
| Lift Vector | More vertical and posterior | Variable; allows more skin redraping in patients with greater laxity |
| Best Candidate | Generally 40s to mid-60s | Mid-60s and older; greater skin laxity requiring more excision |
| Shared Features | Both involve sub-SMAS dissection · Both reposition deep facial soft tissues · Both can achieve excellent results in experienced hands | |
What Does the Scientific Literature Say?
There are three studies in the recent literature worth discussing when comparing deep plane and SMAS facelifts.
This study is interesting because it demonstrates very high levels of satisfaction for both types of facelifts. The satisfaction rate for deep plane facelifts was 94.4% versus 87.8% for the SMAS facelift. Both numbers are high, and honestly that tells you something — when done well, either technique gets patients to a really good place. It is worth noting that this was not a direct head-to-head statistical comparison, so we have to be a little careful about reading too much into the difference between those numbers.
This study looked at complication rates and found that for deep plane and SMAS facelifts, when it comes to bleeding and hematoma formation or nerve injury, the rates are approximately the same between the two techniques.
This paper takes a long-term look at both techniques and ultimately suggests that both are valid approaches — and that it should really come down to surgeon’s choice, level of comfort, and the individual interaction with and assessment of each patient.
In My Experience
I have this thesis that the deep plane facelift and the high SMAS facelift are, in many ways, converging — in terms of what surgeons are actually doing when they call something a deep plane facelift. A lot of proponents of the deep plane facelift are now suggesting entering at multiple points and incorporating some degree of SMAS elevation that comes away from the primary dissection line. The closer that line of elevation moves laterally, the closer what everyone is calling a deep plane facelift is actually becoming a high SMAS facelift. The terminology is blurring.
In the past, when I performed high SMAS facelifts, I actually limited my skin elevation to an extent that was pretty similar to what I and many other surgeons do in a deep plane facelift today. So the idea that a deep plane facelift automatically means less skin elevation is based on a bit of a false premise — it really depends on the surgeon and the patient’s anatomy.
Different techniques may also be more advisable depending on the individual patient. In my experience, a true deep plane facelift with minimal skin elevation works best in younger patients — generally those in the 40 to mid-60s age range. For patients in the mid-60s and older, a high SMAS approach can sometimes be more appropriate. These patients often benefit from slightly more skin elevation, and the skin drapes well with that technique. In a deep plane facelift, the vector and the way the skin drapes tends to be a little more vertical and posterior, which is ideal in many cases — but it also means there is somewhat less skin excision. In older patients who have a greater degree of skin laxity, that additional skin removal that a high SMAS approach allows can be an important advantage.
My preference has settled on the deep plane entry point because it gives me more efficient and direct access to the tissue that most needs to be repositioned, and it allows for more controlled deep tissue movement. That said, none of this terminology debate is ultimately what matters most to a patient. What matters is finding a surgeon who can customize the approach to your anatomy, has real experience with the technique, prioritizes safety, and is someone you can trust — because there may be bumps along the road, and you want someone who’s available and in your corner.
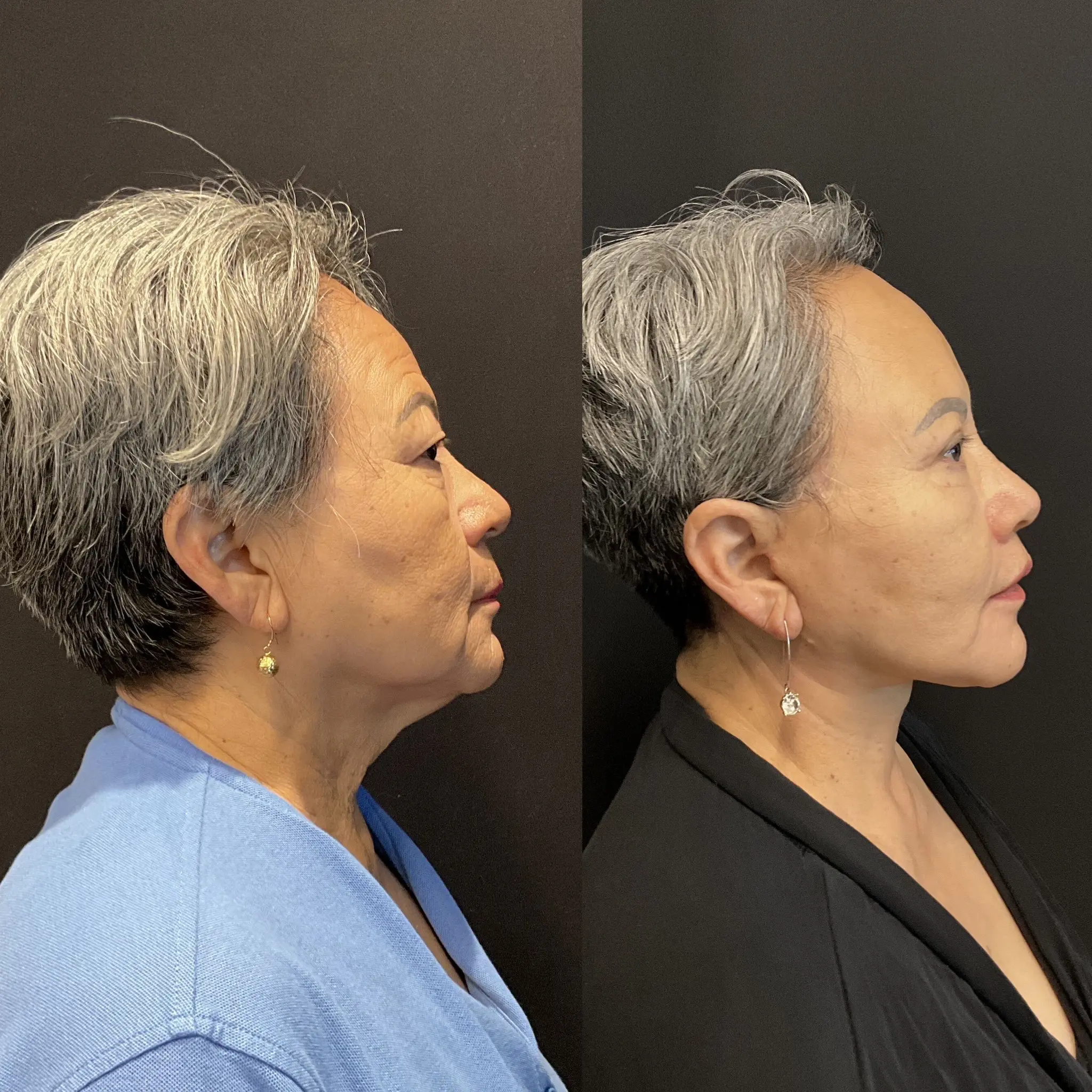
Deep Plane Facelift — Before & After
Patient results. Individual outcomes vary.

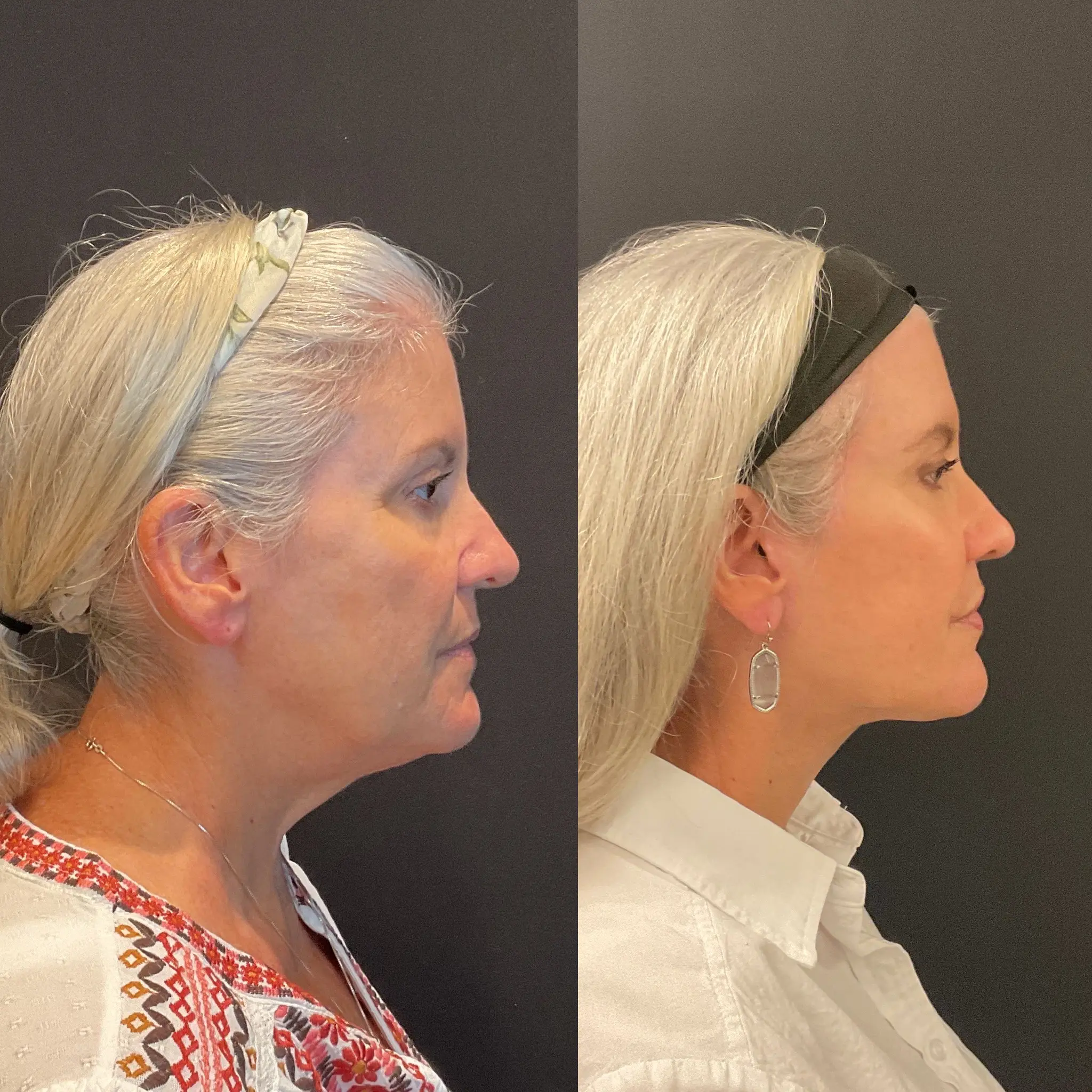
High SMAS Facelift — Before & After
Patient results. Individual outcomes vary.

Frequently Asked Questions
References
- Khoury S, Almubarak Z, Khan H, Boldt G, Villemure-Poliquin N, Nichols AC. The Deep Plane versus SMAS Facelift: A Systematic Review and Meta-Analysis. Aesthetic Plastic Surgery. 2025;49(21):5895–5903. doi: 10.1007/s00266-025-05118-x
- Vayalapra S, Guerero DN, Sandhu V, Happy AA, Imantalab D, Kissoonsingh P, Khajuria A. Comparing the Safety and Efficacy of Superficial Musculoaponeurotic System and Deep Plane Facelift Techniques: A Systematic Review and Meta-Analysis. Annals of Plastic Surgery. 2025;95(5):582–589. doi: 10.1097/SAP.0000000000004454
- Mariani M, Fabbri M, Serra PL, Murone V, Scucchi B, Botti C, Botti G. A Long-Term Evaluation: Deep Plane versus High SMAS Face Lift. Facial Plastic Surgery. 2025;41(5):703–707. doi: 10.1055/a-2510-6495
“`
Want to go deeper on the goals and philosophy behind deep plane facelift surgery?
